We have received numerous questions over the past several weeks regarding the Covid vaccines, and we will try to address most of them in this post. We have compiled this information from different sources which are listed at the end of this piece. Please note, the Pfizer and Moderna COVID-19 vaccines are some of the safest and most effective vaccines for an infectious disease. These vaccines will end this pandemic if almost every human around the world is inoculated.
Will our practice (Allergy, Asthma & Food Allergy Centers) receive vaccines to immunize our patients?
As of 4/28/21, we will NOT as the mRNA approved vaccines require extremely cold temperatures (-70°C or -94°F for Pfizer; -20°C or -4°F for Moderna) for storage, and there is now good access for the general population (except most kids) to receive all 3 approved vaccines.
I have allergies (to foods, drugs, pollens, etc.). Am I at risk for a severe allergic reaction to the vaccine?
If you have an allergy to polyethylene glycol or some injectable medications, you may be at risk, but food allergies, drug allergies to oral medications, and environmental allergies do not put you at any significant risk over the general population. You will also be monitored for at least 15-30 minutes after vaccination, and vaccination sites should have epinephrine on hand on the off chance you have a reaction. Remember, no one has died from Covid vaccination despite millions of doses and as of this post, over 400,000 people have died due to COVID in the US.
There was a recent CDC report with 71% of anaphylaxis cases being in the first 15 min. Anyone with an anaphylactic history can and should wait 30 mins.
There is currently no validated testing for suspected allergy to polyethylene glycol or for other components of the vaccine. You can find more information here: American College of Allergy, Asthma & Immunology (ACAAI) Guidance on Risk of Allergic Reactions to mRNA COVID-19 Vaccines.
Remember, allergic reactions to the vaccine are relatively infrequent; roughly one in every hundred thousand injections — more than 100 times less common than allergic reactions to penicillin. Reactions are being observed because so many people are being immunized. Importantly, everyone who has had a reaction has been effectively treated and stabilized without any long-term problems.
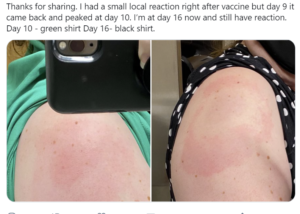
Large local reactions have been reported, especially after Moderna vaccines, including:
- Itching, redness, and swallowing are not uncommon. This comes on late (>5 days from vaccination) and can last for weeks. Treatment is symptomatic: antihistamine, NSAIDs (like ibuprofen)/Tylenol, ice. You CAN still get the second dose! In the Moderna vaccine trial, delayed large locals like these occurred 4 times less with the 2nd dose than the 1st dose.
- Consider switching to the other arm for the second dose if you had a local reaction to the first dose.
- These large local rxns are all very delayed in onset (often after day 8) so mechanistically they are different from immediate reactions.
I’ve heard that the vaccines are made from fetal tissue. Is this true?
NO, the Pfizer and Moderna vaccines are synthetic- made from chemicals. The AstraZeneca (AZ) vaccine (not approved as of 1/25/21) does use an immortalized cell line (HEK 293) derived from an abortive fetus from the 1960s for vaccine production. Here is a commentary that discusses this.
Where can I get information on how to get the Covid vaccination?
- Missouri: covidvaccine.mo.gov/
- Illinois: dph.illinois.gov/covid19/vaccine-faq
- Please also check with the local hospital systems
How do the Covid vaccines work?
COVID-19 vaccines help boost the immune system against the pandemic-causing SARS-CoV-2 virus. As of 1/25/21, two COVID-19 vaccines are available in the U.S. One by Pfizer/BioNTech and the other by Moderna. Both of these utilize messenger RNA (mRNA) to make the spike protein found in the SARS-CoV-2 virus, which attaches to human cells leading to infection. The spike protein stimulates the immune system to make antibodies against this virus, making a person less susceptible to contracting it. Having antibodies against the spike protein can prevent the virus from attaching and infecting human cells. Both vaccines require two doses, three or four weeks apart in order to achieve an optimal immune response.
Are there any safety concerns with the new technologies (mRNA and nanotechnology) being used in the development of COVID-19 vaccines?
There are no known additional risks of mRNA vaccines or lipid nanoparticles. Live attenuated viral vaccines, such as the measles vaccine, induce an immune response that is similar to natural infection. mRNA vaccines, on the other hand, simply give the body instructions to produce one very specific part of a virus – in this case the spike protein – to then induce an immune response. Because mRNA is broken down very quickly in the human body, it is wrapped in a lipid nanoparticle to be able to get into our cells to do its work. Once it gets into the cells to deliver the instructions, the mRNA breaks down very quickly. There are rumors that mRNA vaccines will alter DNA because the RNA molecule can convert information stored in DNA into proteins. That is not true. It is important to note that the mRNA vaccines never enter the nucleus of the cell, where DNA is stored. After injection, the mRNA from the vaccine is released into the cytoplasm of the cells. Once the viral protein is made and on the surface of the cell, mRNA is broken down and the body permanently gets rid of it, making it impossible to change DNA.
This is a nice set of tweets from Andrew Nowalk, MD, Ph.D., a pediatric infectious disease specialist in Pittsburgh. He presents some information on the vaccines that may alleviate some concerns people have about the speed at which the vaccines were developed. They are presented below (but here is a link to his tweets).
- This is NOT a vaccine created in 9 months. The origin goes back many years.
- The first reports of an mRNA vector in a lipid particle used as a transfer vehicle go back to 1989 at the Salk Institute. Vaccines were considered using this in the 1990s. Kariko and Weissman made a big leap forward in 2005.
- They modified the nucleosides of the mRNA, the building blocks that encode the viral protein so that they would be recognized as host RNA and properly translated.
- Moderna (ever notice the last 3 letters) started in 2010 to expressly use this technology.
- The first vaccines of this variety are NOT against #COVID it was MERS and OG SARS. Those trials are more than 3 years old.
- The real analog here is 2009. That’s when we took the pandemic H1N1 strain and made a vaccine with it in 6 months. That’s a good analogy.
- When this vaccine technology and development started, REM and Nirvana were the big bands, Clinton was president, and an i-anything from Apple was more than half a decade away.
Risk of Covid vaccine in context by Aaron E. Carrol, M.D., who is a professor of pediatrics at Indiana University.
What about Covid-19 vaccination in pregnancy?
Please contact your OBGYN to see what his/her current recommendations are. Most OBs are recommending it for pregnant and nursing mothers. The Centers for Disease Control and Prevention (CDC), the American College of Obstetrics and Gynecology (ACOG), and the Society for Maternal-Fetal Medicine agree that the new mRNA COVID-19 vaccines should be offered to pregnant and breastfeeding individuals who are eligible for the vaccine. Here is a piece on the Covid vaccine in pregnancy.
More recently, preliminary findings of a study published in the New England Journal of Medicine on 4/21/21 find COVID-19 mRNA vaccines made by Pfizer and Moderna are safe for pregnant women. A study in JAMA Pediatrics found pregnant women who became infected with the virus were at increased risk for maternal mortality, preeclampsia and preterm birth. Therefore, it is particularly important for those who are pregnant to receive the COVID vaccine, and the CDC now recommends that all pregnant women be vaccinated.
What if I have already had COVID, do I still need the vaccine?
Yes, you should still receive the vaccine. Due to the severe health risks associated with COVID-19 and the fact that reinfection with COVID-19 is possible, you should still be vaccinated.
How soon after being infected from COVID should I get the vaccine?
Current CDC guidelines state you can receive the vaccine as soon as you are fully recovered from symptoms and out of the quarantine period. However, reinfection within 90 days of illness is uncommon, so it may be less critical to get the dose right away. They can wait until closer to the end of the 90 days if they want.
If you were treated for COVID-19 symptoms with monoclonal antibodies or convalescent plasma, you should wait 90 days before getting a COVID-19 vaccine.
The vaccines are not 100% effective, so why should I take them?
The mRNA vaccines are nearly 100% effective against severe illness from COVID-19. Of the 32,000 people in the Pfizer trial, only one developed COVID-19 severe enough to require hospitalization. Beyond the 95% prevention of any clinical COVID-19 infection, the 5% that got the illness had a very minimal illness. So these vaccines are almost totally effective in preventing COVID-19 illness in all qualifying age groups.
If I can still spread the disease after I’ve received the vaccines, why should I take them?
Disease spread was not a specific endpoint in the clinical trials, but if the clinical illness is reduced by 95%, the spread of the virus should also be reduced by 95%. In the Moderna trial, the asymptomatic disease appeared to be as reduced as significantly as symptomatic diseases.
Will the vaccines protect me against the new variants of Covid?
The current data suggest that the vaccines offer varying amounts of protection against the known mutant strains of Covid. While the protection may not reach 95%, it is still very significant.
There are (or will be) different Covid vaccines approved. Which one should I get?
The simplest answer is take whatever vaccine you can get as soon as you can get it since all of the approved (or likely to be approved) vaccines essentially eliminate the risk of a severe Covid infection that will lead to death.
Does the vaccine contain toxic chemicals that will make me sterile?
NO! There are no toxic chemicals in the vaccine. The lipid component is in many foods and cosmetics. The amount of this material you are exposed to every day is hundreds of times more than in the vaccine. All these substances have been shown to be safe in large studies because they are in food and cosmetics. Therefore, it is unlikely that anything in the vaccine would cause a toxic effect.
There are many false rumors about the Covid vaccines, specifically targeting women. Some of them are debunked here.
The information above was compiled from different sources, including:
- James R. Baker, Jr, M.D.
- Aaron E. Carrol, M.D.
- Andy Nowalk, M.D.
- David Stukus, M.D.
- Kimberly Blumenthal, M.D., MSc
Here are more links to frequently asked questions:
- American College of Allergy, Asthma & Immunology Covid FAQ
- Massachusetts General Hospital COVID-19 Vaccine Allergy FAQ
- Pfizer-BioNTech COVID-19 Vaccine Frequently Asked Questions
- Moderna COVID-19 Vaccine Frequently Asked Questions
- Ingredients of the Pfizer Covid vaccine?
- Ingredients of Pfizer and Moderna Covid-19 vaccines
- Other vaccine rumors (and NO, a microchip will NOT be implanted in you when you receive the vaccine)
- How the AstraZeneca vaccine works

